Khác biệt giữa bản sửa đổi của “Vết thương”
←Trang mới: “{{đang dịch 2 (nguồn)}} {{about|wounds in humans and animals|wounds in plants|Plant pathology}} {{Other uses}} {{Infobox Disease | Name = Wound | Image =C…” |
(Không có sự khác biệt)
|
Phiên bản lúc 11:47, ngày 2 tháng 2 năm 2012
Bài viết này là công việc biên dịch đang được tiến hành từ bài viết ArticleName từ một ngôn ngữ khác sang tiếng Việt. Bạn có thể giúp Wikipedia bằng cách hỗ trợ dịch và trau chuốt lối hành văn tiếng Việt theo cẩm nang của Wikipedia. |
| Wound | |
|---|---|
 | |
| Wounded man | |
| Chuyên khoa | y học cấp cứu |
| ICD-10 | T14.0-T14.1 |
| ICD-9-CM | 872-893 |
| MeSH | D014947 |
Vết thương là dạng thương tổn khi da bị rách, cắt hoặc đâm thủng (vết thương hở) hoặc bị tác động bởi một lực gây ra chấn thương (vết thương đóng). Trong bệnh lý, nó được xem là vết thương mạnh gây tổn hại lớp biểu bì da.
Phân loại=
Vết thương hở

Open wounds can be classified according to the object that caused the wound. The types of open wound are:
- Incisions or incised wounds, caused by a clean, sharp-edged object such as a knife, a razor or a glass splinter.
- Lacerations, irregular tear-like wounds caused by some blunt trauma. Lacerations and incisions may appear linear (regular) or stellate (irregular). The term laceration is commonly misused in reference to incisions.
- Abrasions (grazes), superficial wounds in which the topmost layer of the skin (the epidermis) is scraped off. Abrasions are often caused by a sliding fall onto a rough surface.
- Puncture wounds, caused by an object puncturing the skin, such as a nail or needle.
- Penetration wounds, caused by an object such as a knife entering and coming out from the skin .
- Gunshot wounds, caused by a bullet or similar projectile driving into or through the body. There may be two wounds, one at the site of entry and one at the site of exit, generally referred to as a "through-and-through."
Vết thương đóng (chấn thương)
Closed wounds have fewer categories, but are just as dangerous as open wounds. The types of closed wounds are:
- Contusions, more commonly known as bruises, caused by a blunt force trauma that damages tissue under the skin.
- Hematomas, also called a blood tumor, caused by damage to a blood vessel that in turn causes blood to collect under the skin.
- Crush injury, caused by a great or extreme amount of force applied over a long period of time.
-
An open wound
-
A laceration to the leg
-
A lacerated knee
-
An infected puncture wound to the bottom of the forefoot.
-
A puncture wound from playing darts.
Bệnh lý
To heal a wound, the body undertakes a series of actions collectively known as the wound healing process.
Quản lý
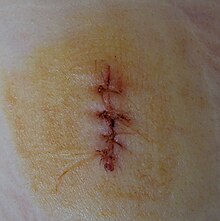
The overall treatment depends on the type, cause, and depth of the wound as well as whether or not other structures beyond the skin (dermis) are involved. Treatment of recent lacerations involves examining, cleaning, and closing the wound. If there is a delay in treatment and the laceration occurred more than 6-24 hours before evaluation, it may be preferable to heal by secondary intention, due to the high rate of infection associated with delayed closure. Minor wounds, like bruises, will heal on their own, with skin discoloration usually disappearing in 1–2 weeks. Abrasions, which are wounds with intact skin (non-penetration through dermis to subcutaneous fat), usually require no active treatment except keeping the area clean, initially with soap and water. Most abrasions tend to have an overall better appearance post-healing when kept moist for about a week with an ointment, such as aquaphor healing ointment or vasoline. Puncture wounds may be prone to infection depending on the depth of penetration. The entry of puncture wound is left open to allow for bacteria or debris to be removed from inside.
Cleaning
For simple lacerations, cleaning can be accomplished using a number of different solutions, including tap water, sterile saline solution, or an antiseptic solution, such as hydrogen peroxide. Infection rates may be lower with the use of tap water in regions where water quality is high.[1] Evidence for the effectiveness of any cleaning of simple wound however is limited.[1] Cleaning of a wound is also known as wound toilet.[2]
Closure
If a person presents to a healthcare center within 6 hours of a laceration they are typically closed immediately after evaluating and cleaning the wound. After this point in time, however, there is a theoretical concern of increased risks of infection if closed immediately.[3] Thus some healthcare providers may delay closure while others may be willing to immediately close up to 24 hours after the injury.[3] A single study has found that using clean non sterile gloves is equivalent to using sterile gloves during wound closure.[4][5]
If closure of a wound is decided upon a number of techniques can be used. These include bandages, a cyanoacrylate glue, staples, and sutures. Absorbable sutures have the benefit over non absorbable sutures of not requiring removal. They are often preferred in children.[6] Buffering the pH of lidocaine makes the freezing less painful.[7]
Dressings
The effectiveness of dressings and creams containing silver to prevent infection or improve healing is not currently supported by evidence.[8]
Antibiotics
Most clean open wounds do not require any antibiotics unless the wound is contaminated or the bacterial cultures are positive. Excess use of antibiotics only leads to resistance and side effects. All open wounds should be cleaned at least twice a day with warm water and soap. Once the wound is cleaned, it should be covered with moist gauze. This should be followed by application of dry gauze and then the wound covered with a bandage. The purpose of a wet to dry dressing allows the bandage to adhere to dead tissue performing a mechanical debridement when removed.This allows new healthy skin to grow and prevents debris from collecting. When the wound is clean, it may be closed with a skin graft. No wound is ever closed if it is suspected to be infected.[9]
Complications
Bacterial infection of wound can impede the healing process and lead to life threatening complications. Scientists at Sheffield University have identified a way of using light to rapidly detect the presence of bacteria. They are developing a portable kit in which specially designed molecules emit a light signal when bound to bacteria. Current laboratory-based detection of bacteria can take hours or even days.[10]
Workup
Individuals who have wounds that are not healing should be investigated to find the causes. Many microbiological agents can be responsible for this. The basic workup includes evaluating the wound, its extent and severity. Cultures are usually obtained both from the wound site and blood. X rays are obtained and a tetanus shot may be administered if there is any doubt about prior vaccination [11]
Chronic
Non-healing wounds of the diabetic foot are considered one of the most significant complications of diabetes, representing a major worldwide medical, social, and economic burden that greatly affects patient quality of life. Almost 24 million Americans—one in every 12—are diabetic and the disease is causing widespread disability and death at an epidemic pace, according to the Centers for Disease Control and Prevention. Of those with diabetes, 6.5 million are estimated to suffer with chronic or non-healing wounds. Associated with inadequate circulation, poorly functioning veins, and immobility, non-healing wounds occur most frequently in the elderly and in people with diabetes—populations that are sharply rising as the nation ages and chronic diseases increase.
Although diabetes can ravage the body in many ways, non-healing ulcers on the feet and lower legs are common outward manifestations of the disease. Also, diabetics often suffer from nerve damage in their feet and legs, allowing small wounds or irritations to develop without awareness. Given the abnormalities of the microvasculature and other side effects of diabetes, these wounds take a long time to heal and require a specialized treatment approach for proper healing.
As many as 25% of diabetic patients will eventually develop foot ulcers, and recurrence within five years is 70%. If not aggressively treated, these wounds can lead to amputations. It is estimated that every 30 seconds a lower limb is amputated somewhere in the world because of a diabetic wound. Amputation often triggers a downward spiral of declining quality of life, frequently leading to disability and death. In fact, only about one third of diabetic amputees will live more than five years, a survival rate equivalent to that of many cancers.
Many of these lower extremity amputations can be prevented through an interdisciplinary approach to treatment involving a variety of advanced therapies and techniques, such as debridement, hyperbaric oxygen treatment therapy, dressing selection, special shoes, and patient education. When wounds persist, a specialized approach is required for healing.[12]
Lịch sử

From the Classical Period to the Medieval Period, the body and the soul were believed to be intimately connected, based on several theories put forth by the philosopher Plato. Wounds on the body were believed to correlate with wounds to the soul and vice versa; wounds were seen as an outward sign of an inward illness. Thus, a man who was wounded physically in a serious way was said to be hindered not only physically but spiritually as well. If the soul was wounded, that wound may also eventually become physically manifest, revealing the true state of the soul.[13] Wounds were also seen as writing on the "tablet" of the body. Wounds acquired in war, for example, told the story of a soldier in a form which all could see and understand, and the wounds of a martyr told the story of their faith.[13]
Xem thêm
Tham khảo
- ^ a b Fernandez R, Griffiths R (2008). Fernandez, Ritin (biên tập). “Water for wound cleansing”. Cochrane Database Syst Rev (1): CD003861. doi:10.1002/14651858.CD003861.pub2. PMID 18254034.
- ^ Simple wound management on patient.co.uk website, viewed 2012-01-08
- ^ a b Eliya, MC (2011 Sep 7). Eliya, Martha C (biên tập). “Primary closure versus delayed closure for non bite traumatic wounds within 24 hours post injury”. Cochrane database of systematic reviews (Online). 9: CD008574. doi:10.1002/14651858.CD008574.pub2. PMID 21901725. Đã bỏ qua tham số không rõ
|coauthors=(gợi ý|author=) (trợ giúp); Kiểm tra giá trị ngày tháng trong:|date=(trợ giúp) - ^ Perelman, VS (1 tháng 3 năm 2004). “Sterile versus nonsterile gloves for repair of uncomplicated lacerations in the emergency department: a randomized controlled trial”. Annals of emergency medicine. 43 (3): 362–70. PMID 14985664. Đã bỏ qua tham số không rõ
|coauthors=(gợi ý|author=) (trợ giúp) - ^ van den Broek, PJ (2011). “[Sterile gloves are necessary in minor surgery]”. Nederlands tijdschrift voor geneeskunde. 155 (18): A3341. PMID 21466736.
- ^ “BestBets: Absorbable sutures in pediatric lacerations”.
- ^ Cepeda MS, Tzortzopoulou A, Thackrey M, Hudcova J, Arora Gandhi P, Schumann R (2010). Tzortzopoulou, Aikaterini (biên tập). “Adjusting the pH of lidocaine for reducing pain on injection”. Cochrane Database Syst Rev. 12 (12): CD006581. doi:10.1002/14651858.CD006581.pub2. PMID 21154371.Quản lý CS1: nhiều tên: danh sách tác giả (liên kết)
- ^ D'Amico G, Pagliaro L, Pietrosi G, Tarantino I (2010). d'Amico, Gennaro (biên tập). “Emergency sclerotherapy versus vasoactive drugs for bleeding oesophageal varices in cirrhotic patients”. Cochrane Database Syst Rev. 3 (3): CD002233. doi:10.1002/14651858.CD002233.pub2. PMID 20238318.Quản lý CS1: nhiều tên: danh sách tác giả (liên kết)
- ^ Wound Infection Signs And Preventive Measures. Retrieved on 2010-01-27
- ^ “Light to detect wound infection” (web). UK scientists have identified a way of using light to rapidly detect the presence of bacteria. bodat. BBC News. 11 tháng 3 năm 2007. Truy cập ngày 17 tháng 3 năm 2008.
- ^ Work Up eMedicine General Surgery. Retrieved on 2010-01-27
- ^ "The Clinical Case for Use of Hyperbaric Oxygen Therapy in the Treatment of Diabetic Wounds," Diversified Clinical Services, copyright 2009
- ^ a b Reichardt, Paul F. (1984). “Gawain and the image of the wound”. PMLA. 99 (2): 154–161. doi:10.2307/462158. JSTOR 462158.
Liên kết ngoài
| Wikiquote có sưu tập danh ngôn về: |
| Tra vết thương trong từ điển mở tiếng Việt Wiktionary |
| Wikimedia Commons có thêm hình ảnh và phương tiện truyền tải về Vết thương. |
- WOUNDS, open-access, print and online, peer-reviewed journal featuring articles about wound care and related research.
- Ostomy Wound Management, open-access, print and online, peer-reviewed journal featuring articles about wound care, ostomy care, incontinence care, and nutrition
- Today's Wound Clinic, the leading journal decision makers read in US wound care clinics.
- Journal of Burns and Wounds, online open-access journal featuring articles about wound care and related research
- Journal of Wound Care, the leading monthly journal for nurses, medics and researchers working in wound care
- US based wound healing society
- Association for the Advancement of Wound Care AAWC
- European Wound Management Association - EWMA works to promote the advancement of education and research.





